“Kidney Disease” found at Creative Commons
Medical advancements over the years are astronomical, saving many patients, including children from several illnesses. Advances have been made to improve survival rates for children with a variety of acute and chronic illnesses, such as cancer, sepsis, cystic fibrosis and congenital heart disease. However, most of these interventions that improve longevity for children living with acute or chronic illness, include the use of nephrotoxic medications. These medications may aid in the advancement of interventions for certain illnesses, but that comes with a price, as they also affect nephrons, which make up the kidneys.
Simply, the kidneys are made up of nephrons, which have two sections, the glomerulus and a tubule. The glomerulus filters your blood and the tubule filters out remaining waste while returning the needed substances to your blood.
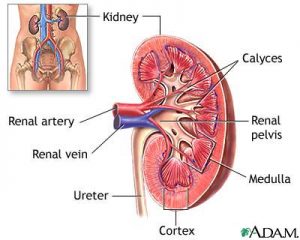
Labelled picture of a kidney. Obtained from Flickr
Although the body can function with one kidney, the role the kidney(s) plays is essential for survival. This study shows that these nephrotoxic medications are very helpful regarding the aid of other illnesses, but they can also be the cause of an acute kidney injury (AKI) or worse, chronic kidney disease (CKD). An injury is sudden and results in a loss of function or other kidney damage, and CKD is gradual kidney failure.
Treatments that use nephrotoxic medications resulted in 10% of adult patients and 40% of pediatric patients following up for CKD after an AKI episode. Therefore, the Acute Disease Quality Initiative recently put into writing that requires active follow-ups for patients after an AKI episode to lower the rate of CKD development afterwards. The vital prevention of AKI or CKD is limiting the use of nephrotoxic medications, especially in children. This study took place in the United Kingdom and found that an increased awareness of these kidney issues in children because of nephrotoxic medications has led to a decrease of use for noncritical illnesses, which in turn aided in a decrease of kidney issues in the pediatric patients.
The study was longitudinal, meaning that they observed patients over a long period of time, in this case 20 years. The doctors followed these children as they
Image of the kidneys in the body. Obtained from Flickr
grew up to determine that impact that nephrotoxic medications played in their health and development. Of the patients that were diagnosed with CKD, 71% of them were exposed to a medication that contained nephrotoxic material, and
50% of children without CKD were exposed as well. These percentages indicate concern for the pediatric CKD community. The reason being that the study found a two-to fourfold higher prescription rate of nephrotoxic medications, despite the knowledge of the risks. Ideally, the prescription rate should have decreased instead, especially given that some of the nephrotoxic medications,
“such as NSAIDs and proton pump inhibitors, have suitable less nephrotoxic alternatives and are therefore potentially avoidable.”
Overall, the awareness of kidney related issues with nephrotoxic medications are essential in children and physicians should try to safely prescribe medications knowing the risk of each medications they prescribe and ensuring that there is not a safer or other suitable treatment that can have the same outcome. By doing this in the case of CKD, physicians can keep children safe from inappropriate prescribing.
Source:
Goldstein, S. (2019). Keep Children with CKD Safe from Inappropriate Prescribing. Clinical Journal Of The American Society Of Nephrology, 15(1), 8-9. doi: 10.2215/cjn.13641119
Alex
"This title was very eye catching! That is so interesting that such a ..."
Alex
"This is really interesting! The fact that crops and plants are damaged is ..."
Alex
"Well done, this article is great and the information is very captivating! Ethics ..."
Alex
"I was intrigued throughout the whole article! This is such an interesting topic, ..."
Alex
"This is such an interesting article, and very relevant!! Great job at explaining ..."
Grandpa
"Honey You Did a good job I will forward to my eye doctor "
murphymv
"This article is fascinating because it delves into the details of the research ..."
murphymv
"I agree, adding the photo helped solidify the main finding. "
murphymv
"This is a fascinating finding. I hope this innovative approach to improving transplants ..."
Sherzilla
"This is a great article! I would really love to hear how exactly ..."
Sherzilla
"It's disappointment that these treatments were not very effective but hopefully other researchers ..."
Sherzilla
"I agree with your idea that we need to shift our focus to ..."
Sherzilla
"It's amazing to see how such an everyday household product such as ..."
Lauren Kageler
"I will be interested to see what the data looks like from the ..."
Lauren Kageler
"A very interesting article that emphasizes one of the many benefits that the ..."
maricha
"Great post! I had known about the plight of Little Browns, but I ..."
Sherzilla
"I assumed cancer patients were more at risk to the virus but I ..."
Sherzilla
"Great article! It sheds light on a topic that everyone is curious about. ..."
maricha
"This article is full of really important and relevant information! I really liked ..."
maricha
"Definitely a very newsworthy article! Nice job explaining the structure of the virus ..."
maricha
"It's interesting to think that humans aren't only species dealing with the global ..."
murphymv
"This is very interesting and well explained. I am not too familiar with ..."
Lauren Kageler
"Great article! This post is sure to be a useful resource for any ..."
Lauren Kageler
"Definitely seems like an odd pairing at first, but any step forward in ..."
murphymv
"What an interesting article! As you say, height and dementia seem unrelated at ..."
murphymv
"Great article! I learned several new methods of wildlife tracking. This seems like ..."
murphymv
"Very interesting topic! You explained cascade testing and its importance very well. I ..."
Alex
"This article is really interesting! What got me hooked right away was the ..."
Sabrina
"I found this article super interesting! It’s crazy how everyday products can cause ..."
Erin Heeschen
"I love the layout of this article; it's very eyecatching! The advancements of prosthetics ..."
murphymv
"Awesome article! I like the personality in the writing. Flash Graphene not only ..."
murphymv
"Very interesting work! I don't know a whole lot about genetics, but this ..."
Cami Meckley
"I think the idea of using virtual reality technology to better help prepare ..."
Erin Heeschen
"I wonder if there's a connection between tourist season and wildfires in the ..."
Ralph berezan
"Not bad Good work "
Michelle
"This sounds like it would be a great tool for medical students! ..."