Children are society’s weakness, we never want them to be harmed, but unfortunately sometimes it is out of our control. Many parents display frustration or confusion because they don’t know why their child is upset, but now they might have an answer. Neonatal diabetes (ND) is a very common illness that is the onset of hyperglycaemia and effects many families but can be very difficult to diagnose at such a young age. The disease tends to present itself within the first six months of a child’s life, however it is possible to be delayed and take up to a year to show. If symptoms occur after the year mark, it is likely that child has Type I diabetes instead.
About 80% of children who have been diagnosed with ND display genetic mutations, which is the most common cause of diabetes in babies.

A picture of DNA, which is what makes up a genome. Image retrieved from Flickr.
However, because the genome is so large, there are constantly new genes being linked to ND, but so far there are more than 20 genes known. A genome is the DNA makeup for our bodies, and each gene on that genome has a specific role that helps many functions throughout the body. Think of it as your body is the country, the genome is the president with all the information, and all the genes are the employees that work for the president to keep everything running smoothly. Therefore, when a mutation occurs and changes a gene, the development and function is affected, which is like an employee forgetting to complete a task and not telling anyone when they realize. The most common mutations that can occur resulting in ND are mutations to the gene that encodes potassium channels in the body or the gene that encodes insulin production
There are many ways that neonatal diabetes can occur, it can be transient, permanent or syndrome ND. Transient diagnosis means that the diabetes will go away but there is a chance of relapse later in life. The permanent diagnosis is when the disease does not remit and continues to manifest therefore requires lifelong treatment. Lastly, syndrome neonatal diabetes is when the child presents with a different syndrome and ND is only a feature of that diagnosis. The most common and effective way of diagnosing ND is using genetic testing to observe the genome and see if there are any mutations to the known affiliate genes. Knowing which gene is mutated also helps doctors with finding the best treatment plan. For instance, there are two genes, KCNJ11 and ABCC8, that if mutated can use sulfonylurea therapy. This therapy is new and uses oral medication and allows majority of the patients (about 90-95%) to be taken off insulin therapy which is great for improving quality of life for patients with permanent ND.
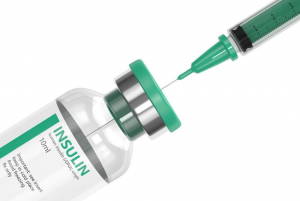
Insulin vial with needle to distribute manually. Image retrieved from Flickr.
Initially, when babies are diagnosed with ND they remain in the hospital for regulation and once the disease in under control they are released to their homes for continued treatment and living. These stays are not very long but can vary depending on the situation. The first thing a doctor does is decrease or eliminate medications, such as epinephrine, that encourage hyperglycemia. Next, if the patient is dehydrated or has electrolyte imbalance, intravenous fluids are administered and monitored to ensure insulin infusion and fluid status remain at healthy levels.
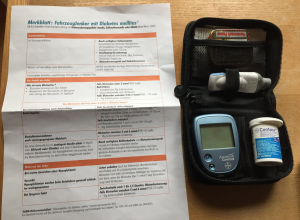
Insulin pump pack. Image retrieved from Flickr.
Once successful, patients transition to insulin therapy, either manually or with a pump. The pump is ideal in infants because sugar levels are monitored constantly and small injections occur as needed. However, due to price the pump may not be possible and parents must monitor their child to test levels regularly and administer insulin if necessary. Once a child grows, the pump becomes a preference and can be used, but most of the time manual administration is preferred and is manageable because the patient becomes old enough to be aware of signs and symptoms of uneven sugar levels.
Source:
Dahl, A., & Kumar, S. (2020). <p>Recent Advances in Neonatal Diabetes</p>. Diabetes, Metabolic Syndrome And Obesity: Targets And Therapy, Volume 13, 355-364. doi: 10.2147/dmso.s198932

Alex
"This title was very eye catching! That is so interesting that such a ..."
Alex
"This is really interesting! The fact that crops and plants are damaged is ..."
Alex
"Well done, this article is great and the information is very captivating! Ethics ..."
Alex
"I was intrigued throughout the whole article! This is such an interesting topic, ..."
Alex
"This is such an interesting article, and very relevant!! Great job at explaining ..."
Grandpa
"Honey You Did a good job I will forward to my eye doctor "
murphymv
"This article is fascinating because it delves into the details of the research ..."
murphymv
"I agree, adding the photo helped solidify the main finding. "
murphymv
"This is a fascinating finding. I hope this innovative approach to improving transplants ..."
Sherzilla
"This is a great article! I would really love to hear how exactly ..."
Sherzilla
"It's disappointment that these treatments were not very effective but hopefully other researchers ..."
Sherzilla
"I agree with your idea that we need to shift our focus to ..."
Sherzilla
"It's amazing to see how such an everyday household product such as ..."
Lauren Kageler
"I will be interested to see what the data looks like from the ..."
Lauren Kageler
"A very interesting article that emphasizes one of the many benefits that the ..."
maricha
"Great post! I had known about the plight of Little Browns, but I ..."
Sherzilla
"I assumed cancer patients were more at risk to the virus but I ..."
Sherzilla
"Great article! It sheds light on a topic that everyone is curious about. ..."
maricha
"This article is full of really important and relevant information! I really liked ..."
maricha
"Definitely a very newsworthy article! Nice job explaining the structure of the virus ..."
maricha
"It's interesting to think that humans aren't only species dealing with the global ..."
murphymv
"This is very interesting and well explained. I am not too familiar with ..."
Lauren Kageler
"Great article! This post is sure to be a useful resource for any ..."
Lauren Kageler
"Definitely seems like an odd pairing at first, but any step forward in ..."
murphymv
"What an interesting article! As you say, height and dementia seem unrelated at ..."
murphymv
"Great article! I learned several new methods of wildlife tracking. This seems like ..."
murphymv
"Very interesting topic! You explained cascade testing and its importance very well. I ..."
Alex
"This article is really interesting! What got me hooked right away was the ..."
Sabrina
"I found this article super interesting! It’s crazy how everyday products can cause ..."
Erin Heeschen
"I love the layout of this article; it's very eyecatching! The advancements of prosthetics ..."
murphymv
"Awesome article! I like the personality in the writing. Flash Graphene not only ..."
murphymv
"Very interesting work! I don't know a whole lot about genetics, but this ..."
Cami Meckley
"I think the idea of using virtual reality technology to better help prepare ..."
Erin Heeschen
"I wonder if there's a connection between tourist season and wildfires in the ..."
Ralph berezan
"Not bad Good work "
Michelle
"This sounds like it would be a great tool for medical students! ..."