Imagine the vascular system in the brain as a strainer used in cooking. After cooking pasta in a pot of water, you pour the pasta over the strainer, so that it catches the noodles, and the water filters out into the sink. Typically, you want a strainer with small holes, so vegetable pieces or meat pieces cooked with your pasta don’t slip out with the water into the sink.
Similarly, specialized cells called pericytes act as the strainer of blood flow in the brain. These cells contribute to forming the blood-brain barrier, which permits nutrients and oxygen to filter through to feed brain cells but prevents toxins from entering the brain. The pericytes play an active role in managing this exchange. Pericytes also regulate blood flow in the small capillary blood vessels. In other words, they determine the width of the blood vessels and decide how much blood can flow freely.
A recent study published in Nature Medicine on February 5th linked pericyte damage with Alzheimer’s Disease and other forms of dementia. Previously, Azheimer’s Disease and other neurodegenerative diseases were associated with accumulations of TAU proteins, toxic proteins that build up over time and inhibit brain function. Researchers at the University of Southern California now think pericytes are to blame as an earlier marker for dementia, causing issues before TAU proteins even show up.
Researchers used a mouse model to simulate pericyte deficiency in humans, and noticed that damaged pericyte cells let some materials leak out of the blood and into the brain that were not supposed to be there, just like a strainer with holes that are too big and macaroni noodles start plopping into the sink. The leaking material was fibrinogen, a protein that creates blood clots at injury sites. During the healing process, fibrinogen is vital, but in the brain, fibrinogen deposits erode away at the insulation barrier of neurons, called myelin, and disrupt electrical communication from one neuron to another. You might equate fibrinogen as the chunks that get through your strainer, and then clog the drain pipe.
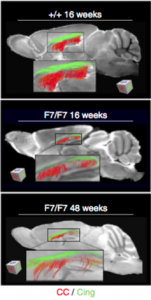
The alarming discovery was that in the absence of healthy pericytes, fibrinogen leaked into the brain, and the cells that produce myelin, called oligodendrocytes, started to die. By the end of the experiment, 50% of the oligodendrocytes were dying or defective. One hypothesis proposed was that besides directly destroying the oligodendrocytes, fibrinogen also blocks oxygen and nutrients from reaching them, further accelerating cell death.
The scientists are hopeful that their research will initiate new treatments for dementia by focusing on the root of the problem: the damaged pericytes producing leaks in the blood-brain barrier. The senior researcher said, “Perhaps focusing on strengthening the blood-brain barrier integrity may be an answer because you can’t eliminate fibrinogen from blood in humans. This protein is necessary in the blood. It just happens to be toxic to the brain.” With future research, the pericytes may become the primary target for dementia treatment and prevention.
Sources:
Montagne, A., Nikolakopoulou, A., Zhao, Z., Sagare, A.P., Si, G., Lazic, D., Barnes, S.R., Daianu, M., Ramanathan, A., Go, A., Lawson, E.J., Wang, Y., Mack, W.J., Thompson, P.M., Schneider, J.A., Varkey, J., Langen, R., Mullins, E., Jacobs, R.E., & Zlokovic, B.V. 2018. Berichte degeneration causes white matter dysfunction in the mouse central nervous system. Nature Medicine [ePub ahead of print].
Vuong, Zang. 2018. Half of all dementias start with damaged ‘gatekeeper cells.’ USC Press Room. Retrieved Feb. 12 from http://pressroom.usc.edu/half-of-all-dementias-start-with-damaged-gatekeeper-cells/.
