May 2021
IV. Essays und autobiografische Texte: Proud of Being a Thai Nurse in the US
Anchalee Dulayathitikul:
“Proud of Being a Thai Nurse
in the United States”
Anna Rosmus, Chesapeake Bay, Maryland
When explorer John Smith traveled up the Chesapeake Bay in 1608, the area was settled by Massawomecks and Susquehannocks. Some locals may (still) find pride in the fact that because of the strategic location at the top of the Bay, Havre de Grace was once considered as capital of the United States. Best known from this area, however, might be John Wilkes Booth, a noted actor from nearby Bel Air, who lamented the abolition of slavery and supported the “Know Nothing” Party, a populist, xenophobic, anti-immigration movement, before he assassinated President Abraham Lincoln in 1865. Decades later, the Bata Shoe Company employed numerous Eastern European refugees at its Belcamp factory. Today, Harford County with its rural and suburban neighborhoods votes predominantly Republican.
According to the 2010 census, Harford had a population of 244,826.[1] After Aberdeen Proving Ground, a U.S. Army facility, University of Maryland Upper Chesapeake Health, a not-for-profit facility with 243 acute care beds,[2] is the county’s biggest employer.
The Covid-19 pandemic highlighted the importance of a functioning medical system. Rarely have people been more grateful for health care workers. Relatively few, however, are aware that immigrants from all over the world form the backbone of our medical care. This article introduces Anchalee Dulayathitikul and a dozen others of international-American identity.
 Photo: Courtesy of Anchalee Dulayathitikul Photo: Courtesy of Anchalee Dulayathitikul |
In March 1988, when Anchalee (AKA Angie) obtained a Bachelor of Science in Nursing and Midwifery at Chiangmai University in northern Thailand, King Bhumibol Adulyadej personally presided over the ceremony.
Asked, whether she studied nursing with the intent of emigration, Dulayathitikul explained how gradually that path evolved:
One of my cousins, who graduated from Chulalongkorn University in Bangkok, worked at a Cambodian refugee camp. How she was helping and coordinating, inspired me to help others as well. We studied in the Thai language. When I was a student nurse, there were a lot of sick people, who needed us. So, I have practiced in as many specialties as I could, from birth to death. Those experiences made me meticulous and dedicated to providing the best care.
Because Thailand is also a tourist destination, we all have seen people from around the world. I always wanted to learn more languages, to better understand and communicate with visitors.
English classes started at 5th grade, and I continued at Catholic high school, but in a small town access was limited. We had no library with English books. Besides our textbook, a Thai-English Dictionary was my only resource. My cousin inspired me to learn more. Every time she visited us, she played guitar, and sang beautiful English songs such as “Donna, Donna” by Joan Baez. That was my first impression of America.
During the Cambodian Civil War, there was a US-Army base in my hometown, and I recall wondering why there were huge radars and so many American soldiers, but there were no resources to get an answer, and local people did not know either.
In 1990, I moved to Bangkok to take an English Class at the American University Alumni Language Center. That and another English institute influenced me the most, regarding America. I practiced speaking English with an American teacher, and I watched American movies. All of that made me wonder what America might look like.
When I decided to take a CGFNS exam, I passed it, but I had no clue what to do with it, and how I could get a job in the United States. So, I remained active as a nurse in Thailand and gained expertise in a renowned hospital. In 2009, I had a chance to visit family members in the USA.
Since then, the soft-spoken nurse recalled traveling annually to the United States, visiting historic parks in various states as an amateur photographer. “When I considered educational opportunities for my own kids,” however, Dulayathitikul said,
I started to gather more details, but high tuition fees would prevent me from sending them to school there. To afford these costs, I was planning to get a job there, and in 2014, I relocated to the States as a permanent resident.
When asked whether she considered other countries, such as the UK, Canada or Australia, the nurse stated, “Not really. I once received an application to become a nurse in the UK, but it was too complicated. Australia is not far from Thailand, but I had no connection or friends there.
Within the United States, the Susquehanna River attracted Dulayathitikul in particular. She liked its surrounding nature and the weather. Looking at the map, she was eying Bel Air, MD, and checked for a hospital.
 |
Information from the University of Maryland Upper Chesapeake Medical Center (UMUCH) website let her perceive this organization as “a big community hospital, accredited by several organizations. Its Intensive Care Unit was accredited by the American Association of Critical-Care Nurses (AACN), and it received a ‘Beacon Award for Excellence’.”
 |
Reza Ostadali,[3] a Chemotherapy Certified Critical Care Nurse, who also teaches at Harford Community College, pointed out, “Most community hospitals cannot do what we do here, even spine and some brain surgeries.”

Photo: Courtesy of Anchalee Dulayathitikul |
“With my extensive critical care background,”[4] Dulayathitikul explained,
this inspired me to get certified there. I have also practiced in a trauma unit and in an emergency surgical unit. Next, I worked in a Medical & Surgical Cardiac Care Unit. While broadening my knowledge of Hemodialysis with the Nephrology Society of Thailand and Thai Nephrology Nurses Association, I attended seminars and an annual academic conference with eight weeks of CABG care in two outstanding Bangkok hospitals. For the last 10 years, I have practiced in the Bangkok Pattaya Hospital, certified by the Joint Commission International. Without English speakers teaching us, however, this was challenging.
 Photo: Courtesy of Anchalee Dulayathitikul Photo: Courtesy of Anchalee Dulayathitikul |
In June 2015, Dulayathitikul began to volunteer at the UMUCH Occupational Health Department. When she applied for a paid position in September, she described herself as a bilingual nurse with basic French, “strong clinical judgement, multitasking, prioritization, critical thinking and problem-solving skills.”
Mark Moody, then Director of Occupational Health, declared that his team is “very successful […] simply because we have highly competent individuals who work very effectively together.” Admitting that “I had some reservations about having a nurse volunteer within the department because I was not sure if it would increase our capacity or even maybe disrupt the normal flow of work,” he did concede that “Angie is the best we could have hoped to have […]. She is a pleasure to work with, and we all hope that she can continue to be a part of the team for as long as she wishes.”
To make that happen, the Thai nurse attended a refresher course for International and U.S. Educated Nurses at Harford Community College. These 148 hours, in turn, included 60 hours of clinical practice at UMUCH.
A Registered Nurse (RN) and adjunct faculty teacher who instructed Dulayathitikul at that time, stated that her
self-assured and calm nature has been a tribute to our clinical experience on 3 East. She is very responsible and never passes up an opportunity to volunteer her services. She has wonderful critical-thinking skills that allow her to anticipate her patients’ needs, communicate effectively to the medical team, patients, and their family. I would highly recommend Anchalee for employment […]. She will be an asset to the organization and the patients she would be providing care to.
Another RN wrote:
I would highly recommend Anchalee Dulayathitikul for any position she is applying for as a professional registered nurse. I have worked closely with Anchalee over the past two months […]. Anchalee has impressed me with her vast knowledge and experience with up-to-date technology, equipment and procedures in the critical care setting. She has worked extensively in a ‘state of the art’ critical care unit in her country [,] which catered a lot to patients traveling internationally to benefit from their services. Anchalee is 100% a team player. […] She is intelligent, diligent, well informed […]. She stands above the others in motivation and a drive to overcome all obstacles in order to meet her career goals. […] Anchalee would be a great asset to any professional nursing team.
UMUCH hired Dulayathitikul as a nurse for its Intermediate Care Unit, where she began to work under the direction of Suzie McHugh, one of the “nurse managers who through their leadership ensure the highest level of quality care to patients and their families.”
Angie, as new colleagues nicknamed the Thai nurse, blended right in.
UMUCH medical staff comes from 58 countries (including USA), and 31% come from abroad.[5] Most of them continue to display a distinct personal attitude shaped by their respective country of origin, even after adapting to US demands and regulations.
Often on the same shift as Angie was CCRN Anna Louise Wilson Gardner, once a record-setting Olympic swimmer from New Zealand, whose parents had worked on their PhDs in the United States, when Anna was born.[6]
A frequent visitor was Dr. Aastha Sethi, a native of India, who speaks English, Hindi, and Punjabi. After graduating from medical school in 2003, the nephrologist with a particularly sunny disposition settled down in Fallston, MD. Camille Henry, a nationally registered PCCN nurse from Guam, affectionately observed that “patients love [Dr. Sethi]. She pays attention to details, always stays on top of things.”
What caught the eye of visitors and health inspectors, time and again, was he level of UMUCH collegiality, especially between medical staff and support staff.[7]
Dr. Abdulla Hussein Abdulla,[8] for example, who graduated from Al Mustansiryia University in Baghdad, Iraq, in 2002, and a female US-colleague were waiting for an elevator to arrive. As the door opened, both hospitalists stepped aside to allow a hostess with an overloaded delivery cart to emerge. Noticing how wobbly the temporary pyramid of piled up food trays became as it crossed the threshold, Abdulla spontaneously clinched his clipboard under one arm and reached under the tip with both hands. Lifting the edible load, he gently asked, “Where may I take those for you, my friend?” With a smile, critical care nurse John Haacke[9] commented, “Abdulla has no ego.”
Kneeling on the floor, before a particularly frail patient on comfort care, was Dr. Kapil Sharma,[10] who graduated from Nepalgunj Medical College in 2004. Asked why he was kneeling, the mild-mannered physician simply stated, “I am tall.”[11]
Quietly stopping under the door frame to peek at a patient with a large tumor and a dire diagnosis was Dr. Muhannad Salah-Al-Deen Kanbour.[12] The hospitalist wondered whether the most recently administered morphine dosage might be wearing off too soon. As the patient slowly opened her eyes, Kanbour handed her his hospital-issued business card. “Call me directly, if a nurse is not coming soon enough,” he encouraged her, “I’ll be there.”
Angie was not surprised.
Kanbour is very respectful. He greets patients every day and asks early on, what they may need. He responds instantly to any changes and treatment will promptly follow. Kanbour also pays close attention to patient complaints. He covers their problems head to toe, including economic hardships, details of insurance plans etc. And he quickly reassesses the situation afterwards.
Josephine Delp, a clinical, clinical training and education expert,[13] whose mother came from England, as a post-WWII bride, added, “Dr. Kanbour is strikingly good at communicating with his patients. Helping them understand their illnesses and the plan he has for their treatment. Very caring.”
In May 2017, Angie’s peers chose her as IMC Nurse of the Year, and in July, the AACN certified her.
 |
Dr. Jason M. Birnbaum joined UMUCH in 2002. Baltimore magazine named him a “Top Doctor” in 2016, and again in 2018, his colleague Josephine Delp called Birnbaum “the best pulmonologist I have ever worked with, a workaholic. He loves what he does, and he is excellent.” When news of a possible pandemic broke, Birnbaum sprang into action. In early March 2020, when UMUCH received its first Covid-19 patient, major sanitation efforts were already underway.
Existing PPE had to be preserved, a lot of additional equipment became necessary, and a vast number of medical staff was to be scheduled for training in the proper use of PAPR.

Photo: Courtesy of Anchalee Dulayathitikul |
The nightshift was barely leaving when Birnbaum already looked after first patients. Slightly nodding, shaking his head, or pointing a hand in silence, he signaled other team members through glass doors when to proceed and when to back off.
Be that in his office next to several elevators or at any desk in ICU and IMC, Birnbaum was nearly constantly seen re-evaluating and writing assessments about infections, neurological, respiratory, cardiological, gastro-intestinal, and renal conditions as well as family situations. During rounds with critical care staff, he addressed these issues Socratically.
Keeping a visibly watchful eye on multiple patients as well was Dr. Hasan Shakoor, a multilingual pulmonologist from Pakistan, who also treats sleep disorders. John Haacke considered Shakoor a “competent” force of nature, humorous but “very focused,” managing “multiple, stressful situations in practical, direct ways.” Baltimore magazine simply named him a “Top Doctor” in 2018.
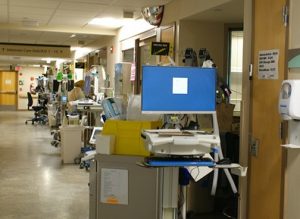 |
Where heavy-duty IV poles,[14] COWs, multiple monitors and other medical equipment lined corridors as far as eyes could see, Dr. Faheem Younus[15] may have been more needed than ever. Unobtrusively meandering his way from one patient to another, Josephine Delp called him her “favorite person, extremely knowledgeable and current. He taught me so much about infectious disease. He truly cares about quality of patient care and is great in working for change.”
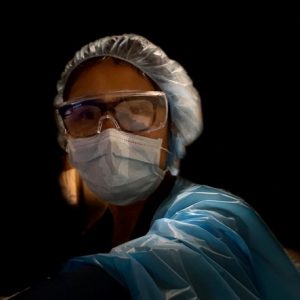 Photo: Courtesy of Anchalee Dulayathitikul Photo: Courtesy of Anchalee Dulayathitikul |
Angie usually worked the nightshift, often alongside Camille Henry, whom John Haacke characterized as “an older nurse, who sees the bigger picture – what a patient needs, aside from medical treatment; maybe kindness.” Also working at night was Dusan Stojanoski, a calm security guard from Macedonia.
Kitchen staff, now working with face masks, served meals for patients in isolation rooms on disposable trays.
 Working the patient line: 22-year old Blake Powell, who started to cook at age 15, and Pradip Gautam[16], a 26-year old dental hygienist from Nepal, who came to the United States in 2014. Working the patient line: 22-year old Blake Powell, who started to cook at age 15, and Pradip Gautam[16], a 26-year old dental hygienist from Nepal, who came to the United States in 2014. |
Unassuming Assefa Beratu, who arrived from Ethiopia in 2016, and Al Johnson, an African-American who grew up in the Baltimore area, were even busier cleaning rooms.
Kingsley Kumi-Poku, a tall, bespectacled lead linen chief, who arrived in the United States from Ghana in 1996, appreciated the fact that Evan Combs, Vice President of Operations at University of Maryland Upper Chesapeake Health, and other senior leaders have personally thanked him for his service.
Few immigrants take that for granted, and fewer yet might be seen for all they bring to the common “table.” Asked, how the Thai culture influenced Dulayathitikul’s being a nurse and an immigrant, she replied:
Thais are famous for smiling. Good characteristics for a Thai also mean being humble and dedicated. Nursing means seeing and treating patients gently, as if they were our own, beloved family members. Caring for them includes hospitality services to their family members.
American people are more independent, and I adjusted [to] my role of caregiver, but I still offer extra care as much as I can, and a patient agrees to.
Asked what Angie liked about community healthcare, she immediately pointed out “a hospital’s support of patients in need of tertiary care, especially its ability to transfer those to higher levels of care.” At UMUCH, she liked how confident the community was in the care provided, and how well it was supported by the team.
Asked what she liked about US healthcare, the Thai nurse marveled at how many people are insured, and thus “less worried or worry-free” if an emergency arises or urgent care was needed. “Supporting facilities or systems such as Acute Rehabilitation,[17] Subacute Rehabilitation, Home Health care, Hospice or Home Hospice care continue to care appropriately for patients and families in need.”
In part, that had to do with areas that differed from her country of origin, where she saw “sufficient and/or adequate medical resources limited by financial means and medical supplies.” What also impressed Angie were “educational opportunities accessible for almost everyone at almost any age.”
Because most people in Thailand have a low income, and government hospitals are the only places to access such services, our healthcare system is far behind the US healthcare system. The numbers of patients always outweigh the numbers of healthcare providers. The workload is high. To provide continuous care to all patients, Thai nurses must offer tender, loving care, be attentive and gentle. Being in that situation, we were instructed to perform selfless care.
What Angie treasured about her own training was that her
Bachelor of Science and Nursing degree included midwifery. Our curriculum contained practice hours for each field, be that medical, surgical, pediatric or ob-gyn. Therefore, we possessed a variety of skilled experiences. Our nursing professors focused on intensive, in-depth care, working hand-in-hand with patients hospitalized in all these fields. The curriculum also allowed us to practice directly under our professors’ supervision and license. This led us indeed to practice compassion, patience, and sacrifice. Without passion for our career, we may not survive on small paychecks.
Today, Angie stated, she is focused on “applying all my knowledge, nursing care strategy, etc. to every patient in UMUCH.” Every day that she experiences with a patient, she is also eager to learn more about UMUCH’s own culture, team and administrative system. “I want to improve and broaden my nursing care spectrum.”
Coming from a country where dedication and skills of individual team members had to bridge gaps in available technology and supplies, she felt “we could do better working team-oriented, not duty-oriented, especially with high acuity patients,” and she is striving to strengthen that teamwork.
If the Thai nurse could, she would cut administrative assignments in favor of more state-of-the-art knowledge in bedside care. To grow in her own professional education, Angie participated in UMUCH educational programs, and she attended academic conferences. To spread this mentality, however, she pointed out it is essential that the employer supports academic growth financially.
Angie would also like to implement a more cost-effective care. Plastic and paper items, for instance, are so readily available that it is not unusual for several boxes of tissues and multiple, still wrapped syringes to be discarded when a patient is discharged. Even cleaning reusable basins seems to require too much of an effort. “With almost everything being disposable here,” Angie commented, “I am wisely spending [on] medical supplies.”
A somewhat sensitive issue was acceptance. Angie recalled that “Trust between patients and me required time.” Especially during her first year, patients questioned her about her country of origin, as well as her knowledge or experience. When called a “Chink,” she replied, “I am a nurse from Thailand with extensive experiences.” Once they were “taken care of by me, however, their attitude turned. Through hard work, I am now accepted and complimented.” Occasionally, Angie’s Thai accent may have created a language barrier, but she also shared memories with patients who have spent time in her homeland.
As a nurse, there was also “no hindrance getting to know my neighbors. I was welcomed. All are happy with my presence, and we help each other. For a couple of months, I actually had a chance to take care of two hospitalized in IMC. They were delighted, and after they returned home, some relatives thanked my family for my care.”
Angie pointed out,
We are all legal immigrants. My daughter adapted a great deal, especially during her first year in school. She is well accepted by classmates and does excel in school. In 2015, she made the Honor Roll. In 2017, she was awarded for artistic excellence by Harford County Public Schools. At the age of 16, she received an Academic Achievement Award. Now, she studies Biomedical Engineer and Forensic Science at Pennsylvania State University.
To support her children’s ongoing education, Angie expected to “be working here until retirement, keeping up with my own knowledge in every single channel I can. I will always love my career and be proud of being a Thai nurse in the United States.”
When one of Angie’s fellow nurses recommended her as hospital-wide Nurse of the Year, she described her not only as a particularly selfless individual but also as one who constantly seeks learning opportunities.
She is always so welcoming to patients, families, and her fellow team members. She takes such care to make each of her patients feel special – her only priority, therefore, [is] embodying the mindset of every patient, every encounter, every day! She is one of the most caring, energetic, hardworking, dedicated and knowledgeable nurses ever encountered. She has not only adapted to the culture in America, but to the culture at U[MUCH] and most especially, the Intermediate Care Unit. […] She has also visited her country recently and shared our practices in America with them and their practices with us.
What the Thai nurse would wish for are opportunities to open the door for other immigrants. Learning from her own experiences, she said, “It is very important, how the supervisor perceives and supports or promotes us. We only need a chance to demonstrate how good we are, and support in directing us.” The same might also apply to multiple other positions, especially in support services, where elaborate language skills, formal degrees, and previous on-site job experiences play only marginal roles.
When a new critical care unit for Covid-19 patients opened, and the first health care workers caught the disease, even some of the most experienced nurses worried about serving 12-hour shifts inside of this cohort unit. After all, some have asthma or diabetes, others have small children or particularly vulnerable spouses. Angie was quickly among those assigned to work there.
Within hours of the unit’s informal opening, walking swiftly through the hallways, came FACHE Lyle Sheldon, the hospital’s president and CEO. Occasionally sitting down at a provider’s computer station, this unassuming, humble, hard-working man pulled out a note pad with hand-scribbled telephone numbers and e-mail addresses, adding latest data to a long list of self-assigned personal tasks.
Quickly catching up with various staff members on their way in and out of individual patient rooms, Sheldon addressed each team member by name, he inquired about the status of a major medical project as well as about minor personal matters. Waving to somebody across the corridor, with an open smile, Sheldon stated, “I am very proud of our international team,” and he freely admitted that “the scope” of operations at this hospital “would not be possible” without its immigrants.
Footnotes:
[1] 81.2% were white, 12.7% black, 2.4% Asian, 0.3% American Indian. 3.5% were of Hispanic origin. 28.1% had German ancestors, 19.8% Irish, 12.2% English, 9.9% Italian, 6.8% Polish, and 6.2% American. For additional details see: “DP02 SELECTED SOCIAL CHARACTERISTICS IN THE UNITED STATES – 2006–2010 American Community Survey 5-Year Estimates”. United States Census Bureau. Retrieved March 25, 2020.
[2] “Licensed Acute Care Beds by Hospital and Service: Maryland, FY 2020 (effective July 1, 2019)”
[3] Ostadali came from Iran in 1978. He recalls his previous work as a personal trainer and credits his wife, a PACU nurse from Scotland, who arrived in the USA in 1984, with his career shift. “It’s not that different,” he explains, “at first I worked with relatively healthy people to keep them out of hospitals, and now I work with critically ill people to get them well enough to leave the hospital.” Ostadali received his BA in science and nursing and his MA in education and nursing. Today, at least three days a week, Ostadali works as a guardian nurse, responding to “codes” and other requests for a rapid response. John Haacke, a critical care nurse whose paternal ancestors lived in northern Germany, freely acknowledges what a good teacher Ostadali is, how helpful and how well he handles stress.
[4] From 1988 until 1990, Dulayathitikul worked as a Registered Nurse at the surgical center of the 2,000 bed Maharaj Nakorn Chang Mai Hospital. After six more years in the Critical Care Unit of Rama 9 Hospital, she served two years at the Phyathai 3 Hospital in Bangkok.
From 1999 until 2005, Dulayathitikul worked at the newly established 150 bed Rajavej Hospital. While she worked in the Intensive Care, Endoscopy, and Recovery Unit, she also helped to establish the Renal Hemodialysis Unit. Dulayathitikul recruited, trained, and supervised new nurses, and a professor who worked with her, deemed her English “above average for the Thai standard.”
From 2005 until 2014, Dulayathitikul was a Registered Nurse at the Critical Care Unit of 400 bed Bangkok Pattaya Hospital, where children and adults with a wide variety of diagnoses which required procedures, such as brain or heart surgery, valve replacements, and cardiovascular thoracic surgery. Dulayathitikul performed basic physical, neurological, and cardiovascular assessments with CAREMAP. She served as a team leader for emergency & disaster codes as well as for the Resuscitation Team. In her recommendation from Pattaya Hospital, we read, that she “collaborated with multidisciplinary team members, worked closely with physicians, nurse assistants, physical therapists, nutritionists to formulate, implement and modify individual care plans.” Equally highlighted was her “ability to remain calm and professional in a fast pace[d] environment with immense experience in interacting over telephone.” She was described as “flexible, adaptable and willing to take on new challenges.” “Excellent organizational and interpersonal communication skills” allowed her to provide “exceptional customer service.” Appreciated were her “effective listening and interpreting skills as to symptoms analysis,” her ability to identify health problems, provide advice in a “warm, compassionate and knowledgeable” manner as well as her cooperation on medical emergency protocols.
[5] Data courtesy of Lyle Sheldon, from May 22, 2020
[6] In 2019, Gardner completed her medical studies and began to work as a nurse practitioner.
[7] UMUCH policy explicitly states, “We are proud of everyone who contributes to the care and services of our patients. Whether it is clinical care and medical services or support staff and facilities management — every team member has an important role in contributing to the health of our community.”
[8] Dr. Abdulla specializes in Emergency Medicine, Hospital Medicine, and Family Medicine. He also speaks Arabic. He accepts Medicare-approved amounts as full payment.
[9] John Haacke recalls working in the ICU at Johns Hopkins University and 15 years at the shock trauma center of the University of Baltimore before he joined UMUCH. This critical care nurse has long-term work experience with all hospital staff that is mentioned in this article and has an expert’s view.
[10] Dr. Sharma speaks Hindi and flawless English. He specializes in Hospital Medicine, Geriatric Medicine, and Internal Medicine.
[11] UMUCH policy demands that providers avoid “towering” over a patient. Especially when explaining test results or treatment options, seeing eye-to-eye at the same height level is actively promoted.
[12] Dr. Kanbour recalls spending a part of his childhood in Germany, where his father, a chemist, was working on his PhD. After Kanbour graduated from the University of Baghdad College of Medicine, in 1996, he specialized in Hospital Medicine and in Internal Medicine. To this day, Kanbour occasionally addresses German-speaking staff and patients in such casual German that some mistake him for a German physician.
[13] Delp, RN, BSN, CNSN, VABC, specialized in inserting and maintaining IV lines of all types for patients throughout the hospital. Until retirement in 2019, her title was Clinical Resource Nurse Vascular Access.
[14] IV poles, or intravenous poles, often have a four or five wheeled base, and two to four hooks on top for bags of fluids. Gravity then ensures a steady drip through hollow plastic tubes, into the veins of a patient.
[15] After graduating from King Edward Medical University in Lahore, Pakistan, in 1995, Younus specialized in infectious diseases and internal medicine. In 2018, Baltimore magazine named Younus, who also speaks Urdu, a “Top Doctor.”
[16] To earn some money while Gautam’s US-born wife is attending college, the couple joined the hospital’s dietary department. “I’ve always loved cooking,” Pradip explains, and “taking care of patients.”
[17] After a traumatic injury, debilitating disease or certain types of surgery, acute rehabilitation provides multidisciplinary programs such as physical, occupational, and speech therapy, in addition to medical management by specially trained physicians.
